Category: ADHD
Is it just me that hides in the toilet at conferences…?
Today, I have been at the British Mecca for Psychiatrists, the annual conference of the Royal College of Psychiatrists. We have taken over the ICC in Birmingham where the entrails of the Tory party conference are still being tidied away. I did have a double take moment of “Lord, I’m at the wrong conference” when I was greeted with the “A Country That Works For Everyone” signage which dwarfed our college’s diminutive logo. The juxtaposition being even greater because within the medical profession, the psychiatrists are probably the most left leaning, our life’s work being in the care of some of the most discriminated and disadvantaged in society who are not usually the Conservative party faithful.
I’m not really a “conference” person. Brown-nosing and networking brings me out in hives, but I have been around long enough to know just enough people to make small talk to. At shrink-fest this usually involves grumbling about:
- Lack of in-patient beds
- Being mistaken for a psychologist
- Not being recognised as “proper doctors”
- Lack of medical students wanting to train in our wonderful specialty
Mostly, I am robust enough to endure colleagues darting-off mid conversation to talk to someone else of greater importance. Occasionally, I bump into old supervisors and I have to admit to them that I’ve chucked in my research and pretend to be blissfully happy about this decision. Other times I catch sight of another female ex-researcher and we indulge in metaphorical hand-holding and sighs of “it’s so hard with children”. If it gets too much, I hide out in the loos checking social media. People post me pictures of dead animals (anti-hunting friends – don’t ask).
It might sound awfully depressing, but I also learnt these amazing nuggets:
From the wonderful Dr Andrea Danese, an Italian contemporary who heads up the Stress Lab at the Institute of Psychiatry. He once gave me a good recipe for pesto and today, he taught me this:
- If you get a nasty cut that gets infected, the skin gets red and “inflamed”. If we took a sample of your blood, we would find raised levels of proteins e.g. C-Reactive Proteins which are called inflammatory markers.
- Stress can cause an inflammatory response, just like an infection in quality but milder. This is to prepare the body to fight stress, in the same way that your body prepares itself to fight an infection.
- Children and adults with depression have raised inflammatory markers.
- These markers are even more raised if there was evidence of early life stress such as childhood maltreatment.
- Adults with raised baseline inflammatory markers are more likely to have recurrent and chronic depression which does not respond to traditional anti-depressant treatments.
- Anti-inflammatory agents usually used as pain killers after surgery (COX-2 inhibitors) have been successful in treating depression, particularly in people with high baseline inflammatory markers.
I know, this sounds dull to you, but to shrinks this is like: Yay! Another drug (cheap too) – maybe they won’t confuse us with psychologists anymore?
I also learnt from Professor Ian Goodyear (Head of Child Psychiatry at Cambridge University) that in his longitudinal studies of depression he divides us parents into the following groups which form a measure of “suboptimal family environment”:
- Optimal (that’s me of course)
- Aberrant (well-meaning but missing in action or clueless)
- Discordant (bickering and self-interested)
- Hazardous (deliberately cruel and abusive)
- Not surprisingly, the majority of children raised by “hazardous” parents end up with all kinds of mental health problems.
And from Professor Eric Taylor, the grand don of my field neuropsychiatry:
- 20-70% of children with ADHD continue to have symptoms into adulthood.
- 50% have another psychiatric diagnosis by age 27 years (mainly anti-social behaviour, drug misuse or depression).
- Children with ADHD with no friends and unsupportive, hostile parents at age 7 years are more likely to develop conduct problems and antisocial behaviour.
- If a child with ADHD lasts to age 17 years without engaging in anti-social behaviour, their parents can heave a large sigh of relief because they will very unlikely ever engage in this type of behaviour (they may still be susceptible to depression unfortunately).
The best part of conference?
The hotel to retire to overnight. Totally kid-free: gym, luxuriating bath, telly, bed and totally guilt-free and legitimate because “I’m working!”.
Roll on day 2!
Managing your child’s behaviour: Can’t behave, Won’t behave?
Over the last few weeks I have been asked by a few people to write something on managing behaviour of children. This is one of the biggest challenges for parents, and yet I had put off writing about this as it is not as easy to give advice on this as it sounds. The “tips” that friends were asking for basically amount to what we in the industry call “behavioural management”. Ways in which parents can magically “change” or “manage” their children’s behaviour. Sadly, there is no magic tip, only all the things that you have already heard of and tried. Behavioural management tries to spell out what is and is not desirable behaviour and strategies try to tip the balance of choice towards behaviours that are desirable. Well known strategies include “the naughty mat” or “time out”, “ignoring” your child’s mild bad behaviour and also the blessed “reward chart”. If you want to read up on behavioural management an excellent book is “The Incredible Years” by Webster-Stratton. I won’t précis what I feel is a thorough account of good behavioural management, but instead ask:
Does behavioural management work?
The answer in theory is unequivocally “yes”.
But, so often in practice is “no”.
This is because behavioural management is easiest to implement when your child is “typical” and has no other problems, and you (the parent) are brilliant, have no problems and are super consistent in everything you do both with your co-parent and school.
Which basically means “no” or only “a bit”– as when does the above situation ever happen?
Here are two reasons why your child may not be “typical”:
Neurodevelopmental problems:
Neurodevelopmental problems, in particular learning difficulty can heavily impact behaviour. In young children, aggression and temper tantrums are typical responses to frustration, but by school age, some control should have been gained over these behaviours. If a child is developmentally delayed, then their ability to behave should be compared to their developmental age rather than chronological age. A 16 year old boy with the developmental level of a 4 year old; can be expected to behave in line with a 4 year old. For a four year old, temper tantrums and hitting out are common responses to frustration, the trouble is that being hit by a 16 year old boy in a temper tantrum has very different consequences to being hit by a 4 year old, and yet, the child “can’t” help responding in this way. These children are often clients in child mental health services as parenting children with severe learning difficulties can be extremely challenging. Other neurodevelopmental disorders also cause behavioural problems. In ADHD children with problems with attention cannot listen to or follow instructions as well as other children. They will tend to act without thinking and may do things that they regret later because they acted without thinking. Children with Autistic Spectrum Disorder may have behavioural problems as they are having difficulty in understanding what is being expected of them and poor social understanding can lead to many more frustrations on a daily basis. Standard behavioural management may not work in these groups of children and behavioural management needs to be adapted to the child’s difficulties. In general it is harder to implement and with more varied results than in children without neurodevelopmental difficulties.
Emotional problems:
Children who are having emotional problems may have difficulties in behaviour. Emotions and behaviour are inextricably linked. When we feel down or stressed out, our behaviour changes. Some of us reach for chocolate, some for alcohol, some people become withdrawn and unsociable, other people become irritable and angry. It is important to assess emotional aspects of your child’s life if their behaviour changes or deteriorates. Children may not always volunteer their states of mind to you. They may not be able to label their emotions, or to express themselves. They may be afraid to talk about these things. Their unhappiness and frustrations are displayed in their behaviour rather than in words. It is your responsibility as a parent to notice, to ask, to label for them, to give them words, to give them permission to talk about their difficulties. To guess and to investigate from asking teachers and friends if nothing is forthcoming. It may be that they are being bullied at school, it may be that they are picking up on the stress in your marriage, it may be something trivial, but if you don’t notice/ enquire, you won’t know and their change in behaviour will just be called “bad behaviour” or “acting out”. In these cases, behavioural management will not work well. Rewards will feel irrelevant, ignoring and punishment will feel like persecution, negative attention will be better than no attention and rejection is a welcome confirmation of their own self-loathing. Finding out what is wrong, offering security will work better here. Unattended emotional problems in children can impact personality and aid development of long-lasting traits that can lead to “bad behaviour” becoming habitual and “part of” a person’s personality that can no longer be easily mended.
In children without these additional problems, the limiting factor to good behaviour is usually the parent not the child.
Lack of sustained motivation:
In the defining clinical trial for children with ADHD where they compared medication to behavioural management (The MTA Study), behavioural management achieved equal outcomes compared to medication. But wait, here the behavioural management programme used highly trained psychologists to work with highly motivated parents and teachers to obtain this outcome. Real-life trials (what we call pragmatic trials) using existing services, which tend not to heavily involve the schools (as the Department of Education is separate from the Department of Health), and non-selected patient groups, that have looked at the efficacy of community parenting and behavioural management programmes have netted unimpressive results. It is not that children’s behaviour cannot be managed; it is that the will of society and parents, is insufficient.
I know this all too well. Big Sis has a weekly spelling test. On the weeks where I have my act together, we sit and learn the words and I test her on the words each day to make sure that at the end of the week, she gets full marks and I reward her for this attainment. This is basically behavioural management in action: co-working towards a set goal that is achievable, achieved and rewarded. This works fantastically well, thumbs up and smiles all around. Once she has done this for a few weeks, I get complacent and I think, well now – maybe I can just give it a skip this week, she and I can both have a relax and we’ll just have a quick look at the words the night before. She gets a couple of mistakes. That’s basically my anecdote for behavioural management. It genuinely works until one day, you can’t be bothered and it all goes a bit wobbly again. The limiting factor is me, not Big Sis.
Parental problems:
Wobbles in my behavioural management can also be seen when I am stressed or distracted. One time when I was very stressed waiting for a phone call regarding a job offer; the children were extremely badly behaved – “for no reason”. I was snappy and shouted at them and they just wouldn’t do what they were told – “it was as if they knew exactly when to wind me up”. Eventually, the phone call came, and I had got the job. That afternoon, they were very well behaved. The change had been in me, and their behaviour merely reflected my state and parenting capability, not something innate in them.
Unrealistic parental expectation:
When we talk about “bad behaviour” we all mean different things and we all have different thresholds as to what is meant by “bad”. Some friends and relatives come by our house and make “tutting” sounds when they see our kids glued to the TV, leave the table at meal times on a whim to dance around the kitchen, bonk each other on the head with cushions and generally shout at each other and at us. To me, this is not bad behaviour – this is just life in our household! Equally, I raise a brow when I see children that never say “please” or “thank you” and run away from their parents on the street, while this is not something that bothers them. When parents complain that their children “Will not do as they are told”, the severity of the issue rather depends on what they are being told to do. If they will not do 60 minutes of piano practice every night, that is rather different from refusing to do their homework, or refusing to stop watching TV; and “good” and “bad” behaviour is sooo dependent on what the parental and school expectation is. Often there are cultural and generational expectations of how children should behave. A normal child in a school with high behavioural expectations may be deemed to have “bad behaviour”, a normal child in one culture may be deemed badly behaved in another. The behaviour is relative and in order to assess behaviour properly, it is important to first evaluate that the expectations are reasonable. There is a limit to how much a child can “change” and they will not bother to attempt to change behaviour if they feel that the bar is being set too high.
Inconsistency:
One of the main saboteurs of a good behavioural management programme is “other people”. The well-intentioned/ or not so well-intentioned other half who disagrees with what you are doing. By not supporting you, they are de facto sabotaging the behavioural management plan because children are such buggers that they can spot disagreement a mile off and work it to their advantage. Much like MPs claiming expenses and benefit fraudsters, they are not averse to trying to get away with as much as they can. Playing one parent off the other must be a favourite game for children. In my opinion parents who want to succeed at behavioural management need to get on board together, or not bother. A similar conundrum exists with the school. If children are told one thing at home and another at school, the “authority” of “the rules” is undermined. It is a good idea when implementing behavioural management to discuss plans with the child’s school so that the same message is delivered to the child.
So in summary, if emotional problems are excluded, behavioural management delivered consistently and well will definitely improve your child’s behaviour, even if they have additional difficulties; but it is by no means a magic wand. It takes hard toil, stamina, guts, persistence and tears, but can reward you with likeable human beings. Isn’t that the essence of parenting?
If you want to know more about behavioural management please buy/ beg/ steal/ borrow: The Incredible Years, by Carolyn Webster-Stratton. This is the programme recommended by my colleague Professor Stephen Scott OBE of the UK’s National Parenting Academy. I have read it cover to cover and it’s good common sense.
References:
Carolyn Webster-Stratton. The Incredible Years. ISBN 978-1-892222-04-06. http://www.incredibleyears.com
The MTA Cooperative Group (1999) A 14-Month Randomized Clinical Trial of Treatment Strategies for Attention-Deficit/Hyperactivity Disorder. Archives of General Psychiatry. 56:1073-1086
How fast is your child’s thinking?
I am posting again on my infant 360 degree appraisal series. Core abilities include memory, attention span, processing speed and impulse control. These are factors that affect ability in all other areas. Deficits in core ability will detrimentally affect ability on the other aspects of function. In this post I will cover processing speed and impulsivity.
Processing speed
Processing speed in the brain is exactly the same as the processing speed of your computer. Some computers are just faster than others. If your computer downloads a movie instantly, while others are still buffering, you can imagine who has the advantage. I remember as a child marveling at my older sister’s ability to do sums in her head while I was still scrambling around for fingers and toes to count. That’s the advantage of processing speed; she was doing the same thing that I was, but just faster and more efficiently and keeping her socks on. Processing speed improves with age in an individual, but there is clearly variation in processing speed between individuals.
Processing speed is all about “how fast” someone can do things. Therefore, in order to test it, you need to know that the child is able to do what you are asking them to do. Tasks chosen should therefore generally be easy. Clinically one measure of processing speed used is a sheet of paper with different symbols on. The child is timed to cross out all the symbols of a particular shape. The score is then based on time taken with a penalty for any false positives (crossed out shapes that were not the specified shape) and false negatives (the correct shape was not crossed out). The task can be varied in difficulty by having all the symbols look very different or very similar. If you are experimentally minded and have an older infant (3 years upwards), you can easily replicate that test at home to gain an idea of processing speed. Here are handy sheets that you can print and use if you are so inclined: Processing Speed Test. Go on, you know you want to, and share with your friends (to find out what their kids score – whilst feigning disinterest of course).
Other simple ways to test processing speed, particularly of younger children include sorting. Sorting items by colour can be mastered easily by an infant and if you time this you can get an idea of the processing speed (again factoring in accuracy). Equally, the time it takes to push shapes through a shape sorter can be used, although this is more of a test for visio-spatial skills, motor skills and processing speed; rather than processing speed alone. Children with good visio-spatial skills and processing speed will be able to do this task quicker. Children that adopt a trial and error approach to the shape-sorter, will get there eventually, but they will be outclassed time wise by someone who is able to process in their head which shape is likely to fit through which hole. Spatial ability is known to predict performance in mathematics and eventual expertise in science, technology and engineering (Tosto, 2014). By the time Lil Bro was one year old, we had acquired so many hand me down toys that we had several shape sorters. The first had only 3 shapes (square, circle and triangle), the second had 10 shapes and the third had about 24 shapes including complex trapeziums and parallelograms. If you are sad like me, you can monitor development through progression of progressively harder shape sorters.
Impulse control/ response inhibition
It is very easy to observe a child’s impulse control, or largely, lack of it! Most adults are able to control their immediate urge to do something to hold out for a greater reward or avoid punishment. For instance, most of us are able to save money in order to buy something big and we are able to wait our turn rather than push into a queue to avoid being told off. Most toddlers are not able to do this, so if you put a new “toy” in front of them, they will try and grab it even if you tell them not to. Try drinking a glass of wine while holding an alert one to two year old in your lap. Good luck.
Sometime between toddler-dom and adulthood, the ability to control impulses develops and strengthens. The earlier that a child develops impulse control, the better they will be perceived, as this will mean that they will be less likely to do things like touch things that they shouldn’t, shout out in class, push in to queues, interrupt other people talking and running across the road without looking. People tend to like children better if they don’t do these things.
You can easily observe your child’s ability to control impulses by taking them into a fancy department store or if you are more daring a china shop. Immediately, you will be telling your child not to touch anything then you can see how long they last. If you really want to test them, you can mix it up a bit. Say “If you don’t touch anything, I’ll buy you some chocolate on the way out” and see if they fare better, or you can up the ante on the temptation and take them to a sweet shop and expect them not to touch! That would be very cruel indeed.
Cruel though is what child psychologists and psychiatrists are in the pursuit of answers, and they actually do this test in the research labs with a cupcake which cannot be eaten despite being left directly in front of the child, on the promise that they will get two cupcakes for leaving it alone. As expected, older children find this easier. This test is very easily replicable at home for anyone who wishes to be so mean (or who has plenty of cupcakes to be eaten)!
Core-ability training
Like for attention, where repeated episodes of bringing back to task and encouraging goal-oriented attention can increase attention span, so too can processing speed, memory and impulse control be improved. The suggested activities for assessing processing speed, memory, impulse control and attention can also be played in order to train infants on these core abilities.
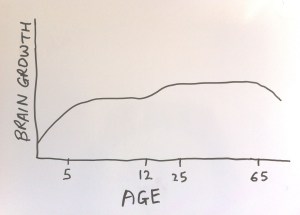
This back of an envelope sketch shows a graph of human brain growth and decline. During infancy the brain is going through massive growth with the child building circuits and connections in the brain in response to its environment at a rapid rate. It is thought that training at this stage in development is likely to physically affect brain development (the interconnections between different parts of the brain) and have larger impact than training at any other time in life. Similarly, continued mental activity (such as playing chess) at the other end of the lifespan can slow the inevitable brain decline in old age by strengthening connections so they are not lost.
There is growing scientific interest in obtaining evidence that attention span and impulse control can be trained. Research into ADHD treatment and prevention are moving towards computer games, aimed at toddlers that will train attention to goal oriented activity (Wass, 2011). Potentially, future ADHD prevention will involve computer-based intervention at infancy rather than medication in childhood. Why wait for a computer game to be developed to do this when parental interaction is much more fun and rewarding. In actuality, many parents are doing this already, only they are doing it instinctively when trying to interact with their child on an activity – encouraging, supporting and helping a child stay focused to complete something fun. Now you can carry on doing these things with the smug knowledge that you are not just passing the time, or playing a game, but also potentially physically improving your child’s brain.
References:
Tosto et al.(2014) Why do spatial abilities predict mathematical performance? Developmental Science (Dev Sci), On-line ahead of print.
Wass et al., Training Attentional Control in Infancy, Current Biology (2011), 21, 1-5.
What is ADHD?
ADHD stands for attention deficit hyperactivity disorder. When I tell people that I am an ADHD specialist, the next question is usually, “What is ADHD anyway?”. It then turns out that the common conception of an ADHD child is of a naughty boy running around the place, and that the common misconception of treatment is of medication to “calm the kid down” or “sedate him”. So to set the record straight, ADHD is primarily a brain disorder that makes focused attention difficult. The hyperactivity is secondary. It is caused partly by genetic factors, and partly by environmental factors. The environmental factors that are important are usually those around pregnancy, birth and early infancy.
I could talk about symptoms and signs, dopamine receptors, synaptic disruption in the fronto-striatal pathways, but you can get that information from any google search. I don’t think that that will help you understand ADHD or its treatment. So instead, I am going to talk about air traffic control. It’s a long analogy, I apologise, but if you bear with me, you will understand more than most medical students about ADHD and its treatment.
You are watching planes at Heathrow airport. The planes are not behaving as they should for some reason. Pilots are circling the landing strips at random, flying very fast at times and almost crashing in an uncontrolled manner. Sometimes multiple planes are attempting to land at once and sometimes planes are adjusting direction and altitude quickly to avert a crash. There doesn’t seem to be any order and the planes will cause a major accident if they don’t slow down. Your first instinct to solve this problem may be to tell all the pilots to reduce their speed. “Pilots, stop being so ‘hyperactive’, slow down!” Sure, that has stopped the pilots whizzing around causing accidents, but it hasn’t improved their ability to land planes. Now, they are slowly and lethargically circling the airport at random. They don’t crash because they are going so slowly, but they don’t do much else either, they don’t know where and when to land.
If you were to go to the air traffic control room and see what was actually happening, you would come up with a better solution. At air traffic control, what you find is that half the staff have disappeared (there is an economic downturn you know), and the remaining staff have been replaced by pimple faced 16 year olds. Each child is looking at 6 screens with two head phones on with pilots shouting at them “Tell me what I do now? What do you want me to do now?” Most of the kids are completely overwhelmed, and banging their heads against the wall. Some are up to the challenge and attempting to land planes, others are shouting random orders based on knee jerk reactions.
Now what is your solution?
From this vantage point, you can clearly see that the pilot’s speed is not the issue. What is the issue is that the control room is ineffective. It is under resourced and has not been taught how to deal with multiple demands on attention and how to organise the information it is getting in order to achieve a goal.
There are 3 options:
1) Re-employ the senior management of the air traffic control room to train the 16 year olds in air traffic control. This will take time, money and a lot of effort. You are still in effect operating with only half the staff, but with time, the senior managers will be able to train the 16 year olds, identify their strengths and weaknesses, motivate and organise them into a team that can effectively manage to land planes, forever. The managers must be committed, able to deal with frustration and most of all, not give up.
2) Call in the cheap immigrant labour from Planet Zog. They will arrive en masse in the morning; land all the planes for you and then blast off in their space ship again at night for next to no money. They only speak Zog, so they cannot train your staff. They also like to pass wind and can make life slightly unpleasant while they are around.
3) Do nothing. Let the situation “muddle through”. There can be two outcomes for this strategy. The 16 year olds may learn slowly from experience and mature into men and women with greater experience and knowledge to be able to land planes on their own. They might crash a few planes, but at the end, emerge mature and competent. Alternatively, the 16 year olds may lose hope. They crash a few planes. Initially by accident. They get lambasted by the press “You useless people, you good for nothing kids. Why can’t you even land a plane?” They crash a few more planes. They decide this is kind of fun, and deliberately crash planes.
Hopefully this will help you to understand that ADHD is primarily a brain disorder, not an “energy” disorder. The control room is the brain, the staff are neural circuitry. The focus in ADHD should be on “Attention deficit”, not the “hyperactivity”.
In ADHD the brain is under functioning, it is unable to organise or prioritise the stimuli it is being constantly fed. It cannot attend to one thought, or follow through on one action, because it is constantly distracted by other thoughts and stimuli. The result is endless non-goal oriented activity; purposeless movement; hyperactivity. Activity itself is not a problem. Endless goal-oriented activity, purposeful movement to multiple demands is multi-tasking, is productivity. Sedation is not the solution. This will slow the brain and body down so that damage will not be caused, but nothing will be actively achieved either. The solutions are:
1) Behavioural management training. This can only realistically be done by parents (with training and support from teachers and psychiatrists/ psychologists). Done well, it can train the child to function at an appropriate level, and motivate them to attend. It is labour intensive, takes time and is expensive. It requires a lot of work and dedication from parents, but can offer long term change. In a randomised clinical trial of behavioural management training against medication, behavioural management produced equal results to medication, few side effects and with longer lasting effects (MTA, 1999). This is why NICE (National Institute of Clinical Excellence in the UK) guidelines suggest behavioural management as first line treatment for ADHD. Unfortunately, much of what the NHS is currently providing in terms of “behavioural management training for ADHD” (if it is even provided) does not match the behavioural management training given in the clinical trial. In pragmatic studies (studies using real life clinics, and unselected patients rather than well-funded research teams with patients recruited for commitment) there is little evidence for benefit of behavioural management. The problem? Cost and parental resources.
2) Medication. This is typically in the form of a stimulant, which stimulates the brain to work. Most of us are already taking a brain stimulant everyday to help with our functioning on a daily basis. Caffeine. Caffeine is in the same class of drugs as methylphenidate (the main ADHD medication), cocaine and amphetamines. Methylphenidate does not cause highs or addiction at doses prescribed in children for ADHD treatment. It can be abused which is why it is a prescription only medication and prescribers will not prescribe it to children whose parents are known drug users. Medication is a cheap and fast solution, but once the medication is stopped, the benefits are also gone. It can sometimes be a good strategy to use medication to allow children to begin participation in behavioural management training. Some children will experience side effects. The tolerability of the side effects is variable between individuals. About 30% of children will not respond to methylphenidate. Good clinicians can get good outcomes from medication prescribing. Bad clinicians; are bad clinicians.
3) Do nothing. Attention levels in the general population increases with age (see my post on attention), and this is no different in children with ADHD. By late adolescence, some children’s attention will have improved to the extent that they no longer fall under the category of having ADHD. By late adolescence the requirement to attend school and formally pay attention for long periods of time is over, and many adolescents with ADHD choose occupations and pastimes that require less focused attention. Thus, their relative attention deficits have less impact on their lives. Only around a third of children progress from childhood ADHD to adult ADHD. However, there is also high downside risk related to the “do nothing” option. We know, that a significant proportion of the “do nothing” group end up being marginalised from school, singled out and scapegoated by parents and teachers and bullied by peers. The impact of these experiences is highly damaging to children and can lead to additional mental health and social problems with more serious consequences than just inattention. ADHD is related to higher rates of conduct disorder, depression, personality disorder, drug abuse and criminality.
Treating ADHD, by whichever method, is not really about “calming children down” as is commonly perceived. It is about allowing potential to be achieved and preventing conduct disorder, depression, personality disorder, drug abuse and criminality.
I know that ADHD is a highly emotive topic for many, so please feel free to air your views.
References:
The MTA Cooperative Group (1999) A 14-Month Randomized Clinical Trial of Treatment Strategies for Attention-Deficit/Hyperactivity Disorder. Archives of General Psychiatry. 56:1073-1086